The frontal nerve is the largest branch of the ophthalmic division, and runs along the roof of the
orbit, bifurcating about midway to the orbital margin into two nerves. name them and what they supply-
orbit, bifurcating about midway to the orbital margin into two nerves. name them and what they supply-
supraorbital and supratrochlear
nerves.
The supraorbital nerve:
- sensation from the mucosa of the frontal sinus
- the skin and conjunctiva of the central part of the upper eyelid
- the skin and pericranium of the anterolateral forehead and scalp as far as the vertex
The supratrochlear nerve :
-sensation from the skin and conjunctiva of the medial part of the upper eyelid
- skin and pericranium of the anteromedial forehead.
nerves.
The supraorbital nerve:
- sensation from the mucosa of the frontal sinus
- the skin and conjunctiva of the central part of the upper eyelid
- the skin and pericranium of the anterolateral forehead and scalp as far as the vertex
The supratrochlear nerve :
-sensation from the skin and conjunctiva of the medial part of the upper eyelid
- skin and pericranium of the anteromedial forehead.
whtat is otalgia ?
direct causes?
indireckt=
direct causes?
indireckt=
pain in ear
Common causes of otalgia may be direct;
• acute otitis externa
• acute otitis media
• Perichondritis
• trauma
• Herpes zoster infection (Ramsay Hunt syndrome)
- tumour
indirect causes:
• Tonsillitis
• Dental disease
• TMJ dysfunction
• Cervical spine disease
• Cancer of the pharynx and/or larynx
Common causes of otalgia may be direct;
• acute otitis externa
• acute otitis media
• Perichondritis
• trauma
• Herpes zoster infection (Ramsay Hunt syndrome)
- tumour
indirect causes:
• Tonsillitis
• Dental disease
• TMJ dysfunction
• Cervical spine disease
• Cancer of the pharynx and/or larynx
what is otorrhea?
what does a mucoid discharge indicate?
what is does chronic but scanty offensive discharge indicate?
sudden onset of bleading?
acute bleeding?
what does a mucoid discharge indicate?
what is does chronic but scanty offensive discharge indicate?
sudden onset of bleading?
acute bleeding?
discharge
can be mucopurulent, serous or bloodstained
perforation of the tympanic membrane associated with infection of the middle ear.
cholesteatoma where infected keratin forms in a pocket behind the tympanic membrane.
malignant change.
Acute bleeding following trauma would indicate that the two are related. Severe trauma may fracture the
temporal bone, and may be associated with leakage of watery CSF.
can be mucopurulent, serous or bloodstained
perforation of the tympanic membrane associated with infection of the middle ear.
cholesteatoma where infected keratin forms in a pocket behind the tympanic membrane.
malignant change.
Acute bleeding following trauma would indicate that the two are related. Severe trauma may fracture the
temporal bone, and may be associated with leakage of watery CSF.
what does a flush of blood vessel over the handle of malleus indicate?
what does a bright red tympanic membrane indicate?
what does an acute effusion indicte, which woudl be visible behind the tympanic membane?
what does aute otitis media produce?
what is glue ear? grommet?
what does dysfunction of the pharyngotympanic tube indicate?
what does a bright red tympanic membrane indicate?
what does an acute effusion indicte, which woudl be visible behind the tympanic membane?
what does aute otitis media produce?
what is glue ear? grommet?
what does dysfunction of the pharyngotympanic tube indicate?
e early otitis media,
advanced stage if the tympanic membrane appears
bright red.
acute upper respiratory tract infection.
Acute otitis media typically produces a mucopurulent fluid in the middle ear, which will release by perforating the tympanic
membrane and producing a copious discharge
.
Persistence of the effusion may lead to its thickening,
commonly known as ‘glue ear’. A grommet may be
visible if this has been treated surgically.
Dysfunction of the pharyngotympanic tube may cause absorption of the air in the middle ear and retraction of the tympanic membrane. This will give undue prominence to the short lateral
process of malleus, while a Valsalva manoeuvre on the part of the patient should produce outward movement of the tympanic membrane and a ‘popping’ of the ears.
advanced stage if the tympanic membrane appears
bright red.
acute upper respiratory tract infection.
Acute otitis media typically produces a mucopurulent fluid in the middle ear, which will release by perforating the tympanic
membrane and producing a copious discharge
.
Persistence of the effusion may lead to its thickening,
commonly known as ‘glue ear’. A grommet may be
visible if this has been treated surgically.
Dysfunction of the pharyngotympanic tube may cause absorption of the air in the middle ear and retraction of the tympanic membrane. This will give undue prominence to the short lateral
process of malleus, while a Valsalva manoeuvre on the part of the patient should produce outward movement of the tympanic membrane and a ‘popping’ of the ears.
what is the wishpered voice test?
- carried out behind the patient, out of field of view to avoid lipreading.
-Mask hearing in the contralateral ear by rubbing the tragus, and ask the patient to
repeat a combination of letters and numbers, initially at 15cm with a normal speaking voice,
then at arms-length (~60cm), then at arms-length at a whisper
- The latter should be at about
30dB and is considered normal. T
-Mask hearing in the contralateral ear by rubbing the tragus, and ask the patient to
repeat a combination of letters and numbers, initially at 15cm with a normal speaking voice,
then at arms-length (~60cm), then at arms-length at a whisper
- The latter should be at about
30dB and is considered normal. T
what is the webers test?
- Strike the fork to produce a note and place the base on the patient’s
vertex, or in the middle of his/her forehead.
• If hearing is normal, or if hearing loss is symmetrical, the noise will
be heard in the middle, or equally in both ears.
• If hearing loss is due to a conductive problem in one ear, sound
will be loudest in that ear – since other, external sounds are not
• If hearing loss is sensorineural, the sound will be loudest in the unaffected ear.
Clarification of type of hearing loss requires Rinne’s
test.
vertex, or in the middle of his/her forehead.
• If hearing is normal, or if hearing loss is symmetrical, the noise will
be heard in the middle, or equally in both ears.
• If hearing loss is due to a conductive problem in one ear, sound
will be loudest in that ear – since other, external sounds are not
• If hearing loss is sensorineural, the sound will be loudest in the unaffected ear.
Clarification of type of hearing loss requires Rinne’s
test.
what is rinnes test?
- folk on patient’s mastoid processes.
-Ask them to signal when they can no longer hear the note.
I- mmediately move the tuning fork away from the mastoid process, to the external auditory meatus on the same side, and ask the patient if they can hear the tuning fork now.
if so, the indication is that air conduction is better than bone conduction (AC > BC)
and there is no conductive deafness.
A negative Rinne’s test is when conductive deafness is present – bone conduction is better than
air conduction (BC > AC). An exception, however, is when one ear has no hearing at all. The
test may be falsely negative as sound is conducted through the bones of the skull to the ‘good’
ear.
-Ask them to signal when they can no longer hear the note.
I- mmediately move the tuning fork away from the mastoid process, to the external auditory meatus on the same side, and ask the patient if they can hear the tuning fork now.
if so, the indication is that air conduction is better than bone conduction (AC > BC)
and there is no conductive deafness.
A negative Rinne’s test is when conductive deafness is present – bone conduction is better than
air conduction (BC > AC). An exception, however, is when one ear has no hearing at all. The
test may be falsely negative as sound is conducted through the bones of the skull to the ‘good’
ear.
what is the dix hallpike positional test?
what does it diagnose?
what does it diagnose?
- otoconia of the utricular macule may become dislodged and over time relocated to one of the semicircular ducts (usually the posterior).
-The otoconial debris within the semicircular duct
causes abnormal endolymph displacement and a sensation of
vertigo known as benign paroxysmal positional vertigo, which
may be diagnosed with a Dix-Hallpike Positional Test
• Ask the patient to sit upright on an examination couch, with
their head turned 45° to one side.
• Rapidly lower the patient until their supported head is
angled 30° below horizontal over the top edge of the couch
(or place a pillow for the upper back).
• Ask the patient to keep their eyes open and report any
feelings of vertigo.
• Examine the eyes for nystagmus – BPPV may have a
latent period of up to 20s before vertigo commences,
accompanied by an inferolateral rotary nystagmus which
will fatigue (adapt).
• Repeat the test with the patient’s head turned 45° to the
other side.
BPPV may be mimicked by Ménière’s disease, vestibular
neuritis, head injuries and brain tumours. Central pathologies such as cerebrovascular disease
and MS tend to produce an immediate nystagmus that shows no adaptation.
what is the fistula test?
Repeated occlusion of the external auditory meatus by compression of the tragus may produce
a sense of imbalance or vertigo which is suggestive of an abnormal communication (= fistula)
between the middle ear and vestibular apparatus, e.g. erosion due to cholesteatoma
a sense of imbalance or vertigo which is suggestive of an abnormal communication (= fistula)
between the middle ear and vestibular apparatus, e.g. erosion due to cholesteatoma
what does compression mean?
rarefaction?
what is ampllitude?
with what is it measured?
rarefaction?
what is ampllitude?
with what is it measured?
compression (increased pressure) and rarefaction (reduced pressure)
The pressure differential is the amplitude
of a sound wave, which is proportional to loudness, measured with a logarithmic decibel (dB)
scale.
how is pressure transmitted via the ovale window? more celarly, though which fulid in which structure wirst, and then though what sturcture and though waht fluid and sturcte back to the round window?
pressure wave is transmitted to the perilymph within the scala vestibuli of the cochlea.
Since the outer wall of the scala vestibuli is incompressible bone, the pressure wave within is
forced to dissipate through the perilymph either towards the helicotrema and back to the
secondary tympanic membrane at the round window, or, more usually, across the delicate
vestibular membrane and the cochlear duct to the basilar membrane and overlying spiral organ
Since the outer wall of the scala vestibuli is incompressible bone, the pressure wave within is
forced to dissipate through the perilymph either towards the helicotrema and back to the
secondary tympanic membrane at the round window, or, more usually, across the delicate
vestibular membrane and the cochlear duct to the basilar membrane and overlying spiral organ
the saccule and utricle contain what structre?
what does it do?
what das the utricular ? do?
the saccular ??
what ist he ? composed of?
what do they connect with?
what does it do?
what das the utricular ? do?
the saccular ??
what ist he ? composed of?
what do they connect with?
macula
which signals head position (in relation to the trunk).
responds to centrifugal and vertical acceleration,
responds to linear acceleration.
columnar supporting cells
between which are interspersed mechanoreceptive hair cells, similar to those found in the spiral organ of the cochlea.
It is these macular hair cells that a proportion of vestibular nerve
endings connect with, either almost enclosing the cell (goblet or type I hair cell), or by a small
dendritic connection (columnar or type II hair cell).
which signals head position (in relation to the trunk).
responds to centrifugal and vertical acceleration,
responds to linear acceleration.
columnar supporting cells
between which are interspersed mechanoreceptive hair cells, similar to those found in the spiral organ of the cochlea.
It is these macular hair cells that a proportion of vestibular nerve
endings connect with, either almost enclosing the cell (goblet or type I hair cell), or by a small
dendritic connection (columnar or type II hair cell).
when the head is moved form a position of equilibrium , what happens? 4
1. the gelatinous membrane and embedded otoconia tend to move with respect to the receptor cells, causing
bending of the stereocilia and stretching of the tiplinks, which are associated with ion channels
2. hair cells have a basal level of activity, generating action potentials at a constant rate from the associated vestibular nerve endings.
3. Deflection of the stereocilia towards the kinocilium will depolarize (excite) the hair cell membrane and increase the frequency of action potentials; deflection away from the kinocilium will hyperpolarize (inhibit) the hair cell
membrane and reduce the frequency of action potentials.
4. Varied orientations of the hair cells within the utricular and saccular maculae allows the brain to accurately determine the direction
of gravity and the position of the head.
bending of the stereocilia and stretching of the tiplinks, which are associated with ion channels
2. hair cells have a basal level of activity, generating action potentials at a constant rate from the associated vestibular nerve endings.
3. Deflection of the stereocilia towards the kinocilium will depolarize (excite) the hair cell membrane and increase the frequency of action potentials; deflection away from the kinocilium will hyperpolarize (inhibit) the hair cell
membrane and reduce the frequency of action potentials.
4. Varied orientations of the hair cells within the utricular and saccular maculae allows the brain to accurately determine the direction
of gravity and the position of the head.
the ampulla contains a sensory crest. what is its name?
what is the cupula?
what is the cupula?
crista
ampullaris.
Type I and II hair cells are interspersed in a columnar epithelium of
support cells, and their stereocilia and kinocilia are embedded in an overlying ridge of gelatinous glycoprotein known as the
cupula.
ampullaris.
Type I and II hair cells are interspersed in a columnar epithelium of
support cells, and their stereocilia and kinocilia are embedded in an overlying ridge of gelatinous glycoprotein known as the
cupula.
the pharyngotympanic tube connects the middle ear to what structure?
the frist third of the tube is made up of what and the rest?
with what is the tube lined?
what it the tubes function?
how can the tube be opened?
the frist third of the tube is made up of what and the rest?
with what is the tube lined?
what it the tubes function?
how can the tube be opened?
nasal meatus of the nasopharynx
. The first third of the tube is bony and the remainder cartilaginous, and the entire
tube is lined with mucous membrane continuous with that of the middle ear and the nasopharynx.
The pharyngotympanic tube functions to equalize pressure within the middle ear with atmospheric pressure (in the nasopharynx) and thus allow free movement of the tympanic
membrane.
,
and the tube needs to be actively opened by contraction of muscles of the soft palate (levator veli palatini and tensor veli palatini). This is usually achieved during yawning or swallowing.
. The first third of the tube is bony and the remainder cartilaginous, and the entire
tube is lined with mucous membrane continuous with that of the middle ear and the nasopharynx.
The pharyngotympanic tube functions to equalize pressure within the middle ear with atmospheric pressure (in the nasopharynx) and thus allow free movement of the tympanic
membrane.
,
and the tube needs to be actively opened by contraction of muscles of the soft palate (levator veli palatini and tensor veli palatini). This is usually achieved during yawning or swallowing.
list the two muscles of the middle ear.
what is their function?
where do they originate from?
what does each one do?
what are their innervations?
what is their function?
where do they originate from?
what does each one do?
what are their innervations?
tensor tympani and stapedius
-act to dampen movements of the auditory ossicles, and tensor tympani also dampens vibration of the tympanic membrane.
Tensor tympani originates from the superior surface of the cartilaginous part of the pharyngotympanic tube, the greater wing of the sphenoid and the petrous part of the temporal
bone, and inserts onto the handle of the malleus.
- acts to pull the handle medially, thereby tensing the tympanic membrane and reducing the amplitude of its oscillations, and in this way preventing damage to the internal ear by loud sounds.
- stapedius tendon emerges from a tiny foramen at the apex of the eminence and inserts onto the neck of the stapes.
- acts to pull the stapes posteriorly and tilt its base
(footplate) in the oval window, tightening the annular ligament by which the ossicle is attached, and thereby reducing the oscillatory range.
- prevents excessive movement of stapes.
stapedius: the nerve to stapedius, a branch of the facial nerve
tensor tympani: is supplied by the motor root of the
trigeminal nerve running with its mandibular division (V3).
-act to dampen movements of the auditory ossicles, and tensor tympani also dampens vibration of the tympanic membrane.
Tensor tympani originates from the superior surface of the cartilaginous part of the pharyngotympanic tube, the greater wing of the sphenoid and the petrous part of the temporal
bone, and inserts onto the handle of the malleus.
- acts to pull the handle medially, thereby tensing the tympanic membrane and reducing the amplitude of its oscillations, and in this way preventing damage to the internal ear by loud sounds.
- stapedius tendon emerges from a tiny foramen at the apex of the eminence and inserts onto the neck of the stapes.
- acts to pull the stapes posteriorly and tilt its base
(footplate) in the oval window, tightening the annular ligament by which the ossicle is attached, and thereby reducing the oscillatory range.
- prevents excessive movement of stapes.
stapedius: the nerve to stapedius, a branch of the facial nerve
tensor tympani: is supplied by the motor root of the
trigeminal nerve running with its mandibular division (V3).
list the blood supply of the middle ear 5
where to the veins drain to?
where does the lymph drain to?
where to the veins drain to?
where does the lymph drain to?
- branches from the ascending pharyngeal artery,
a branch of the external carotid,
the middle meningeal artery
artery of the pterygoid canal,
both branches of the maxillary artery.
Veins drain into the pterygoid plexus.
Drainage of lymph from the middle ear is to the parotid lymph nodes.
a branch of the external carotid,
the middle meningeal artery
artery of the pterygoid canal,
both branches of the maxillary artery.
Veins drain into the pterygoid plexus.
Drainage of lymph from the middle ear is to the parotid lymph nodes.
where can we ding the internal ear.
of what 2 structures does it consist of.
of what 2 structures does it consist of.
within the petrous part of the temporal bone
bony labyrinth (a series of cavities within the bone containing
perilymph) and a membranous labyrinth (a series of endolymph*-filled membranous sacs
and ducts suspended within the bony labyrinth). This constitutes the vestibulocochlear organ
concerned with the reception of sound and the maintenance of balance.
bony labyrinth (a series of cavities within the bone containing
perilymph) and a membranous labyrinth (a series of endolymph*-filled membranous sacs
and ducts suspended within the bony labyrinth). This constitutes the vestibulocochlear organ
concerned with the reception of sound and the maintenance of balance.
the cochlea is concerend with what?
where does the spiral duct begin?
what is the modolius?
what is the promontory?
after the basal turn, wich what space does the bony labyrinth commmunicate?
where does the spiral duct begin?
what is the modolius?
what is the promontory?
after the basal turn, wich what space does the bony labyrinth commmunicate?
hearing
The spiral canal of the cochlea begins at the vestibule
contains canals for blood vessels and branches of the cochlear nerve. T
the large basal turn of the cochlea protrudes into the tympanic cavity as the promontory of the labyrinthine (medial) wall.
subarachnoid space, just superior to the jugular foramen, through a cochlear aqueduct.
The spiral canal of the cochlea begins at the vestibule
contains canals for blood vessels and branches of the cochlear nerve. T
the large basal turn of the cochlea protrudes into the tympanic cavity as the promontory of the labyrinthine (medial) wall.
subarachnoid space, just superior to the jugular foramen, through a cochlear aqueduct.
what is the vestibule?
what does its lateral wall contain?
what does the vestibule contain ?2
what does its lateral wall contain?
what does the vestibule contain ?2
small ovale chamber behind the chochle.
lateral wall contains the oval window
(fenestra vestibuli), occupied by the base
of the stapes and its annular ligament,
and the round window (fenestra
cochleae), closed by the secondary
tympanic membrane.
The vestibule contains two sacs, the utricle and
saccule of the membranous labyrinth.
lateral wall contains the oval window
(fenestra vestibuli), occupied by the base
of the stapes and its annular ligament,
and the round window (fenestra
cochleae), closed by the secondary
tympanic membrane.
The vestibule contains two sacs, the utricle and
saccule of the membranous labyrinth.
there are three semicircular canals (suoerior, lateral and posterior). they open into vestibule by five orifices.
what do they sense?
what does the superior sc sense?
what does the posterior semicicular canal sense?
what does the lateral semicircular canal sense?
what do the canals contain?
what do they sense?
what does the superior sc sense?
what does the posterior semicicular canal sense?
what does the lateral semicircular canal sense?
what do the canals contain?
senses nodding ('pitching') movements of the
head.
lateral rotational movements ('rolling') of
the head (as in cartwheeling)
the lateral semicircular canal sensing rotations of the head around a vertical axis ('yawing', as in pirouetting).
The canals contain the semicircular ducts of the membranous labyrinth.
head.
lateral rotational movements ('rolling') of
the head (as in cartwheeling)
the lateral semicircular canal sensing rotations of the head around a vertical axis ('yawing', as in pirouetting).
The canals contain the semicircular ducts of the membranous labyrinth.
movements of the linkd tips of stereocilia causes their membranes to depolarise. what neurotransmitter do they release?
what happens next?
what happens next?
neurotransmitter glutamate from the hair cell,
glutamte bidns to sensory neurons that synapse on each hair cell -> Generated action potentials travel in axons to their neuronal cell bodies in the spiral ganglion -> cochlear nerve, a component of the vestibulocochlear (VIII) cranial nerve ->deforming waves ascend and then descend in the neighbouring scalae vestibuli and tympani -> Pressure waves descending in the scala tympani are converted (back) to vibrations at the secondary tympanic membrane of the round window and dissipated in the air of the tympanic cavity.
glutamte bidns to sensory neurons that synapse on each hair cell -> Generated action potentials travel in axons to their neuronal cell bodies in the spiral ganglion -> cochlear nerve, a component of the vestibulocochlear (VIII) cranial nerve ->deforming waves ascend and then descend in the neighbouring scalae vestibuli and tympani -> Pressure waves descending in the scala tympani are converted (back) to vibrations at the secondary tympanic membrane of the round window and dissipated in the air of the tympanic cavity.
what is the ductur reuniens?
the utricle communicates with the saccule through which duct?
this duct gives rise to a side branch,. name it.
this side branch emerges from the bestibular aqueduct as what structure and contains what?
what is maculae?
macuale contains mechanoreceptice hair cells, they are innervated by what erve? what information do they convey?
the utricle communicates with the saccule through which duct?
this duct gives rise to a side branch,. name it.
this side branch emerges from the bestibular aqueduct as what structure and contains what?
what is maculae?
macuale contains mechanoreceptice hair cells, they are innervated by what erve? what information do they convey?
The saccule is continuous with the cochlear duct via the ductus reuniens
utriculosaccular duct,
the endolymphatic duct
The endolymphatic duct emerges from the vestibular aqueduct as the endolymphatic sac, a small reservoir for excess endolymph
The utricle and saccule both contain specialised areas of sensory epithelium called maculae.
Mechanoreceptive hair cells in these areas are innervated by the vestibular nerve, and convey
sensations of centrifugal and vertical acceleration from the utricle, and linear acceleration
from the saccule.
utriculosaccular duct,
the endolymphatic duct
The endolymphatic duct emerges from the vestibular aqueduct as the endolymphatic sac, a small reservoir for excess endolymph
The utricle and saccule both contain specialised areas of sensory epithelium called maculae.
Mechanoreceptive hair cells in these areas are innervated by the vestibular nerve, and convey
sensations of centrifugal and vertical acceleration from the utricle, and linear acceleration
from the saccule.
list the blood suppply of the internal ear. the bony labyrinth is suppplied by what three branches?
membranous labyrinth?
with which two nerves does it enter the acoustic meatus?
to what three brancehs does it give reise to and what do tehy supply?
membranous labyrinth?
with which two nerves does it enter the acoustic meatus?
to what three brancehs does it give reise to and what do tehy supply?
1 anterior tympanic branch of the maxillary
artery,
2 a stylomastoid branch of the posterior auricular artery
3 petrosal branch of the middle meningeal artery.
1 labyrinthine artery, which may be a branch of the
anterior inferior cerebellar artery,
It enters the internal acoustic meatus with the facial (VII) and glossopharyngeal (IX) nerves
1 cochlear branch,
2,3 vestibular branches, which
supply the vestibular apparatus.
artery,
2 a stylomastoid branch of the posterior auricular artery
3 petrosal branch of the middle meningeal artery.
1 labyrinthine artery, which may be a branch of the
anterior inferior cerebellar artery,
It enters the internal acoustic meatus with the facial (VII) and glossopharyngeal (IX) nerves
1 cochlear branch,
2,3 vestibular branches, which
supply the vestibular apparatus.

1 utricle
2 footplate of stapes occupying the ovale window
3 utricosaccular duct
4 round window
5 ductus reuniens
6 scala tympani
7 cochlear duct
8 scala vestibuli
9 helioctrema
10 saccule
11 dura mater
12 endolympahatic duct
13 superior semicircular duct
14 ampulla
15 posterior semicircular duct
16 lateral semicircular duct
2 footplate of stapes occupying the ovale window
3 utricosaccular duct
4 round window
5 ductus reuniens
6 scala tympani
7 cochlear duct
8 scala vestibuli
9 helioctrema
10 saccule
11 dura mater
12 endolympahatic duct
13 superior semicircular duct
14 ampulla
15 posterior semicircular duct
16 lateral semicircular duct
what are the three extrinsic muscle that attach pina to skull?
by what nerve is it supplied also the inner ones?
by what nerve is it supplied also the inner ones?
Small, extrinsic ligaments and muscles (the anterior, superior and posterior auricular muscles)
attach the pinna to the skull
shape. All of these muscles are innervated by branches of the facial nerve.
attach the pinna to the skull
shape. All of these muscles are innervated by branches of the facial nerve.
list the innercation sensory to pinna ( 5)
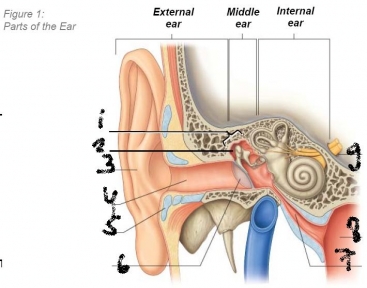
The sensory innervation of the pinna is from many sources (see Figure 1.1):
• Superficially by the great auricular, lesser occipital and the auriculotemporal branch
of the mandibular division of the trigeminal nerve
• Deep branches of the vagus and facial nerves
• Superficially by the great auricular, lesser occipital and the auriculotemporal branch
of the mandibular division of the trigeminal nerve
• Deep branches of the vagus and facial nerves
list the arterial supply of the pinna. 3 out of 1
lymphatic drainage from anteior part to where?
posteriorl?
lymphatic drainage from anteior part to where?
posteriorl?
The arterial supply of the pinna is from various branches of the external carotid artery, i.e. the
superficial temporal, occipital and posterior auricular arteries.
Lymphatic drainage passes anteriorly to the superficial parotid nodes, posteriorly to the mastoid nodes, and sometimes to the upper deep cervical and the superficial cervical
lymph nodes
superficial temporal, occipital and posterior auricular arteries.
Lymphatic drainage passes anteriorly to the superficial parotid nodes, posteriorly to the mastoid nodes, and sometimes to the upper deep cervical and the superficial cervical
lymph nodes
what is auicular haematoma?
what can it result in?
what can it result in?
Bleeding within the auricle is known as an auricular haematoma, where blood collects between the perichondrium and auricular cartilage, distorting the contours of the auricle.
As a haematoma develops it may increasingly
compromise the blood supply to the cartilage, and, if untreated, result in fibrosis and
permanent deformation of the auricle (e.g. the cauliflower or boxer’s ear found in many
professional fighters).
As a haematoma develops it may increasingly
compromise the blood supply to the cartilage, and, if untreated, result in fibrosis and
permanent deformation of the auricle (e.g. the cauliflower or boxer’s ear found in many
professional fighters).
what is cerumen?
how is it produced?
why is it there?
how is it produced?
why is it there?
The part of the canal nearest the outside is made of cartilage covered with skin that produces cerumen (wax) from modified sweat glands (ceruminous glands).
Small hairs in the canal, with the wax, provide a barrier to dust, pollen and other
small foreign bodies.
Small hairs in the canal, with the wax, provide a barrier to dust, pollen and other
small foreign bodies.
what strutures does the tympanic membrane seperate?
what is the membarne made up from? 3 layers
what is the membarne made up from? 3 layers
The tympanic membrane separates the middle ear from the external auditory meatus.
The membrane is made up of a thin outer squamous epithelial layer (continuous with the skin of
the external auditory meatus),
a middle layer of fibrous connective tissue
an inner mucosal layer (continuous with that lining the tympanic cavity of the
middle ear).
The membrane is made up of a thin outer squamous epithelial layer (continuous with the skin of
the external auditory meatus),
a middle layer of fibrous connective tissue
an inner mucosal layer (continuous with that lining the tympanic cavity of the
middle ear).
what is tympanic membrane perforation?
what causes it?
treatment=
what causes it?
treatment=
oitis media(infeection)
m
foreign bodies in the external acoustic meatus
excessive pressure (e.g. during
scuba diving, although this is usually secondary to infection)
Most ruptures tend to heal spontaneously, but surgical intervention may be necessary if the tear is large. Occasionally it may be
necessary to surgically enter the middle ear through the tympanic membrane (myringotomy), e.g. to
release pus from a middle ear abscess. As the chorda tympani nerve, blood vessels and the ossicles are
associated with the upper half of the tympanic membrane, incisions are usually made posteroinferiorly
m
foreign bodies in the external acoustic meatus
excessive pressure (e.g. during
scuba diving, although this is usually secondary to infection)
Most ruptures tend to heal spontaneously, but surgical intervention may be necessary if the tear is large. Occasionally it may be
necessary to surgically enter the middle ear through the tympanic membrane (myringotomy), e.g. to
release pus from a middle ear abscess. As the chorda tympani nerve, blood vessels and the ossicles are
associated with the upper half of the tympanic membrane, incisions are usually made posteroinferiorly
how is the middle ear also called?
where is it?
what does it contain (4)
what do they do?
any attachments?
where is it?
what does it contain (4)
what do they do?
any attachments?
tympanic cavity)
within the petrous part of the
temporal bone.
It contains the auditory ossicles – the malleus (L. hammer), incus (L. anvil)
and stapes (L. stirrup) through which sound is conducted. The malleus is attached to the
tympanic membrane and articulates with the incus, which in turn articulates with the stapes
within the petrous part of the
temporal bone.
It contains the auditory ossicles – the malleus (L. hammer), incus (L. anvil)
and stapes (L. stirrup) through which sound is conducted. The malleus is attached to the
tympanic membrane and articulates with the incus, which in turn articulates with the stapes
the tmpanic cavity has many walls, list the anterior one.
The superior tegmental wall is formed by a thin plate of bone, the tegmen tympani, which also forms the anterior surface of the petrous part of the temporal bone and separates the
tympanic cavity from the dura mater of the floor of the middle cranial fossa.
tympanic cavity from the dura mater of the floor of the middle cranial fossa.
list the inferior jugular wall of the tympanic cavity.
layer of bone overlying the superior bulb of the
internal jugular vein. Occasionally this wall is thickened by the presence of mastoid air
cells. Near the medial border of the floor is a small aperture through which the tympanic
branch of the glossopharyngeal nerve (IX) enters the middle ear.
internal jugular vein. Occasionally this wall is thickened by the presence of mastoid air
cells. Near the medial border of the floor is a small aperture through which the tympanic
branch of the glossopharyngeal nerve (IX) enters the middle ear.
list the anterior wall of the TC.
Its inferior part consists of a thin layer of bone
separating the tympanic cavity from the internal carotid artery, and the superior part is
deficient due to the presence of a large opening to the pharyngotympanic tube and a smaller
housing the canal of the tensor tympani muscle.
separating the tympanic cavity from the internal carotid artery, and the superior part is
deficient due to the presence of a large opening to the pharyngotympanic tube and a smaller
housing the canal of the tensor tympani muscle.
explaint he posterior wall.
inferior part :
-a bony partition between the tympanic cavity and mastoid air cells. Superiorly:
- the epitympanic recess is continuous with the aditus (L. entrance, access) to the mastoid antrum, connecting the tympanic cavity to the mastoid air cells.
The canal containing the facial nerve descends between the mastoid wall and the antrum, medial to the aditus (the mastoid antrum (L. cave), is a common cavity within the mastoid process of the temporal bone into which mastoid air
cells open.
-a bony partition between the tympanic cavity and mastoid air cells. Superiorly:
- the epitympanic recess is continuous with the aditus (L. entrance, access) to the mastoid antrum, connecting the tympanic cavity to the mastoid air cells.
The canal containing the facial nerve descends between the mastoid wall and the antrum, medial to the aditus (the mastoid antrum (L. cave), is a common cavity within the mastoid process of the temporal bone into which mastoid air
cells open.
what is mastoiditis?
what is its danger?
treatment?
what is its danger?
treatment?
Mastoiditis is an inflammation of the antrum and air cells within the mastoid process, usually
secondary to a middle ear infection (otitis media).
There is a danger of the infection spreading
through the petrosquamous fissure to cause osteomyelitis within the tegmen tympani, and/or
meningitis in the middle cranial fossa. Mastoiditis can usually be dealt with using antibiotics, but
occasionally pus within the mastoid air cells may require draining. Surgical access can be achieved,
especially in young children, through the antrum, although care must be taken not to damage the facial
nerve in its course through the mastoid wall of the tympanic cavity.
secondary to a middle ear infection (otitis media).
There is a danger of the infection spreading
through the petrosquamous fissure to cause osteomyelitis within the tegmen tympani, and/or
meningitis in the middle cranial fossa. Mastoiditis can usually be dealt with using antibiotics, but
occasionally pus within the mastoid air cells may require draining. Surgical access can be achieved,
especially in young children, through the antrum, although care must be taken not to damage the facial
nerve in its course through the mastoid wall of the tympanic cavity.

1 aditus to mastoid formane
2 ovale window
3 pyramidal eminence
4 chorda tympani nerve
5 facial nerve
6 internal jugular vein
7 tympanic branch of glossopharyngeal nerve
8 chorda tympani nerve
9 internal carotid artery
10 sympathetic plexus
11 branch form internal carotid plexus
12 lesser petrosal
13 eustachian tube
14 tensor tympani
15 tegen tympani
16 promontory
17 prominence of facial canal
18 prominence of lateral semicircular canal
2 ovale window
3 pyramidal eminence
4 chorda tympani nerve
5 facial nerve
6 internal jugular vein
7 tympanic branch of glossopharyngeal nerve
8 chorda tympani nerve
9 internal carotid artery
10 sympathetic plexus
11 branch form internal carotid plexus
12 lesser petrosal
13 eustachian tube
14 tensor tympani
15 tegen tympani
16 promontory
17 prominence of facial canal
18 prominence of lateral semicircular canal
list the featrues of the medial wall of the TC.
- The medial labyrinthine wall separates the middle and internal ear, i.e. it also forms the
lateral wall of the internal ear
- oval and round windows provide communication between
the middle and internal ear
- The basal coil of the cochlea forms a rounded promontory
- bulging into the tympanic cavity from this wall, and its overlying mucous membrane is associated with a tympanic plexus
lateral wall of the internal ear
- oval and round windows provide communication between
the middle and internal ear
- The basal coil of the cochlea forms a rounded promontory
- bulging into the tympanic cavity from this wall, and its overlying mucous membrane is associated with a tympanic plexus
what are the principal contributers to the tympanic plexus?
what does it innervate?
what does it innervate?
The principal contributors to this plexus are
the tympanic branch of the glossopharyngeal nerve (IX) and branches from the internal
carotid plexus,
it innervates the mucous membrane of the middle ear, the mastoid area and the pharyngotympanic tube. The lesser petrosal nerve leaves the plexus and travels across the anterior surface of the petrous part of the temporal bone, eventually to leave the
middle cranial fossa through the foramen ovale and enter the otic ganglion.
the tympanic branch of the glossopharyngeal nerve (IX) and branches from the internal
carotid plexus,
it innervates the mucous membrane of the middle ear, the mastoid area and the pharyngotympanic tube. The lesser petrosal nerve leaves the plexus and travels across the anterior surface of the petrous part of the temporal bone, eventually to leave the
middle cranial fossa through the foramen ovale and enter the otic ganglion.
desribe the lateral wall of the TC.
6The lateral membranous wall is almost entirely formed from the peaked convexity of the
(primary) tympanic membrane, but also, superiorly, by the bony wall of the epitympanic
recess. The handle of the malleus is attached to the tympanic membrane, while its head
extends into the epitympanic recess.
(primary) tympanic membrane, but also, superiorly, by the bony wall of the epitympanic
recess. The handle of the malleus is attached to the tympanic membrane, while its head
extends into the epitympanic recess.
the nasociliary nerve is with the lacrimal and frontal the three divison of v1. The nasociliary nerve divides within the orbit into three branches. name them.
Tposterior ethmoidal, anterior ethmoidal and
infratrochlear nerves.
post. ethmodial: spenoid sinus and post. ethmoidal cells
ant ethmoidal: ant cranial fossa, nasal caviy, lower 1/2 nouse
infrotrochlar nerve (its termination) : medial art of upper and lower eyelids
lacrimal say
skin of upper half of nouse
medail conjunctiva
external nasal (continuation of an. ethmoidal: skin inside nosue and septum.
infratrochlear nerves.
post. ethmodial: spenoid sinus and post. ethmoidal cells
ant ethmoidal: ant cranial fossa, nasal caviy, lower 1/2 nouse
infrotrochlar nerve (its termination) : medial art of upper and lower eyelids
lacrimal say
skin of upper half of nouse
medail conjunctiva
external nasal (continuation of an. ethmoidal: skin inside nosue and septum.
The lacrimal nerve is the smallest branch of the ophthalmic division. It is primarily a cutaneous
nerve. what does it supply?
nerve. what does it supply?
small area of skin and conjunctiva of the lateral part of the
upper eyelid, but also contains some secretomotor fibres from a communicating branch of the
zygomaticotemporal nerve that innervate the lacrimal gland.
upper eyelid, but also contains some secretomotor fibres from a communicating branch of the
zygomaticotemporal nerve that innervate the lacrimal gland.
The maxillary division of the trigeminal nerve passes anteriorly in the dura mater of the lateral
wall of the cavernous sinus, just inferior to the ophthalmic division, and leaves the cranial cavity
through the foramen rotundum to enter the pterygopalatine fossa. which branches does it give off?,
wall of the cavernous sinus, just inferior to the ophthalmic division, and leaves the cranial cavity
through the foramen rotundum to enter the pterygopalatine fossa. which branches does it give off?,
-gives off branches to the pterygopalatine ganglion
-continues anteriorly to enter the orbit through the inferior
orbital fissure
- Within the orbit the maxillary division divides into its terminal branches - the
zygomatic and infraorbital nerves.
-continues anteriorly to enter the orbit through the inferior
orbital fissure
- Within the orbit the maxillary division divides into its terminal branches - the
zygomatic and infraorbital nerves.
The zygomatic nerve runs to the lateral wall of the orbit and gives rise to the smaller two nereves. name them and what they supply.
• The zygomaticofacial nerve traverses the zygomaticofacial canal in the zygomatic bone
at the inferolateral angle of the orbit and receives cutaneous sensation from the skin on
the prominence of the cheek.
• The zygomaticotemporal nerve sends a communicating branch, containing secretomotor
fibres, to the lacrimal nerve within the orbit and then passes through the
zygomaticotemporal canal in the zygomatic bone to the temporal fossa and receives
cutaneous sensation from the skin of the anterior part of the temporal fossa.
The infraorbital nerve continues in the infraorbital groove and canal, where it gives rise to which branches? emerges though which foramen? it divides ti which branches after emerging form this foramen?
-superior alveolar branches receiving sensation from the teeth of the upper jaw
- palatine branches receiving sensation from the palate
- branches to the mucosa of the maxillary
It emerges from the infraorbital foramen and immediately divides into inferior palpebral, internal and external nasal and superior labial branches receiving sensation from the skin and
conjunctiva of the lower eyelid, the anteroinferior nasal septum and skin of the cheek and
lateral nose and the skin and oral mucosa of the upper lip, respectively
- palatine branches receiving sensation from the palate
- branches to the mucosa of the maxillary
It emerges from the infraorbital foramen and immediately divides into inferior palpebral, internal and external nasal and superior labial branches receiving sensation from the skin and
conjunctiva of the lower eyelid, the anteroinferior nasal septum and skin of the cheek and
lateral nose and the skin and oral mucosa of the upper lip, respectively
what is trigeminal neuralgia?
in which age group does it happen?
with which v division is it assocaited?
cause?
treatment?
in which age group does it happen?
with which v division is it assocaited?
cause?
treatment?
Trigeminal neuralgia (or tic doloreux∗) is a disorder of the sensory root of the trigeminal nerve
most common in middle-aged and elderly people
associated with the maxillary division (less frequently in the
mandibular division and least in the ophthalmic division)
.
The cause of trigeminal neuralgia is unknown, but may be due to an aberrant blood vessel
-surgical displacement of such vessels has relieved symptoms. -temporary block of the infraorbital nerve by
injection of alcohol.
- branches of the infraorbital nerve may be surgically transected or
avulsed at the foramen, or ablated using selective radio frequencies from a needle electrode passed
through the foramen ovale.
- sensory root may be partially cut between the ganglion and pons
(rhizotomy), or the spinal tract sectioned (tractotomy). S
most common in middle-aged and elderly people
associated with the maxillary division (less frequently in the
mandibular division and least in the ophthalmic division)
.
The cause of trigeminal neuralgia is unknown, but may be due to an aberrant blood vessel
-surgical displacement of such vessels has relieved symptoms. -temporary block of the infraorbital nerve by
injection of alcohol.
- branches of the infraorbital nerve may be surgically transected or
avulsed at the foramen, or ablated using selective radio frequencies from a needle electrode passed
through the foramen ovale.
- sensory root may be partially cut between the ganglion and pons
(rhizotomy), or the spinal tract sectioned (tractotomy). S
what is special about the mandibular division?
what are the sensory branches (3)?
what do they supply ?
from what embryonic structure do they derive from?
what nerves does the main trunk of v3 give off (2)?
what does the big trunk finally divide into?
what are the sensory branches (3)?
what do they supply ?
from what embryonic structure do they derive from?
what nerves does the main trunk of v3 give off (2)?
what does the big trunk finally divide into?
the only division of the trigeminal nerve to contain a
motor component.
It has three sensory branches (auriculotemporal, buccal and mental) that supply the area of skin derived from the embryonic mandibular prominence, and also supplies
motor fibres to the muscles of mastication (temporalis, masseter, medial and lateral
pterygoids) as well as the tensor tympani, tensor veli palatini, the anterior belly of
digastric and the mylohyoid muscles.
derived form embryonic madnibular division.
The main trunk of the mandibular division gives off two branches; a meningeal branch which supplies the meninges in the middle cranial fossa, and a branch to the medial pterygoid
muscle, which gives off two further branches to the tensor tympani and tensor veli palatini
muscles.
As the main trunk of the mandibular division descends, it divides into a small anterior and a
large posterior part.
motor component.
It has three sensory branches (auriculotemporal, buccal and mental) that supply the area of skin derived from the embryonic mandibular prominence, and also supplies
motor fibres to the muscles of mastication (temporalis, masseter, medial and lateral
pterygoids) as well as the tensor tympani, tensor veli palatini, the anterior belly of
digastric and the mylohyoid muscles.
derived form embryonic madnibular division.
The main trunk of the mandibular division gives off two branches; a meningeal branch which supplies the meninges in the middle cranial fossa, and a branch to the medial pterygoid
muscle, which gives off two further branches to the tensor tympani and tensor veli palatini
muscles.
As the main trunk of the mandibular division descends, it divides into a small anterior and a
large posterior part.
the anterior part gives rise to three motor braches and one sensory branch. name them
The anterior part gives rise to three motor branches and one sensory branch;
• The masseteric nerve runs laterally to innervate the masseter muscle
• Two deep temporal nerves run superiorly to enter the deep surface of temporalis
• The nerve to the lateral pterygoid muscle enters its deep surface
• The buccal nerve runs anteriorly and emerges from beneath the anterior border of the
masseter. It receives sensation from the skin over the cheek and the mucous
membrane lining the cheek (
• The masseteric nerve runs laterally to innervate the masseter muscle
• Two deep temporal nerves run superiorly to enter the deep surface of temporalis
• The nerve to the lateral pterygoid muscle enters its deep surface
• The buccal nerve runs anteriorly and emerges from beneath the anterior border of the
masseter. It receives sensation from the skin over the cheek and the mucous
membrane lining the cheek (
the posterior part gives rise to two sesnory bracnhes and one mixes branch. name them.
• The auriculotemporal nerve . It receives cutaneous sensation from the skin of the auricle, external auditory meatus,
tympanic membrane, parotid gland and the scalp of the temporal region, but also
receives postganglionic parasympathetic secretomotor fibres from the otic ganglion,
which it conveys to the parotid gland.
• The lingual nerve runs anteroinferiorly in front of the inferior alveolar nerve. At the
lower border of the lateral pterygoid muscle it is joined by the chorda tympani nerve,
and often a branch from the inferior alveolar nerve. It receives sensation from the
anterior two thirds of the tongue.
• The inferior alveolar nerve descends on the lateral surface of the sphenomandibular
ligament and then enters the mandibular canal and runs anteriorly below the
mandibular teeth, from which it receives sensation. It emerges through the mental foramen as the mental nerve to receive cutaneous sensation from the chin, lower face
and lower lip. Just before it enters the mandibular foramen, the inferior alveolar nerve gives rise to the mylohyoid nerve which supplies the mylohyoid muscle and the
anterior belly of the digastric muscle.
what does the parotid gland supply?
sensory?
parotid sheath and overlying skin?
parasympathetic component?
sympathetic?
sensory?
parotid sheath and overlying skin?
parasympathetic component?
sympathetic?
- auriculotemporal branch of the mandibular division of the
trigeminal nerve,
- the great auricular nerve, a branch of the cervical plexus composed of fibres from the anterior rami of C2 and C3, innervates the parotid sheath and overlying skin
-The parasympathetic component of the glossopharyngeal nerve (CN IX) supplies presynaptic
secretory fibres to the otic ganglion and post-synaptic parasympathetic fibres are
conveyed from the ganglion to the gland within the auriculotemporal nerve
- sympathetic comes form cervical ganglia through the external carotid nerve plexus on the external carotid artery.
trigeminal nerve,
- the great auricular nerve, a branch of the cervical plexus composed of fibres from the anterior rami of C2 and C3, innervates the parotid sheath and overlying skin
-The parasympathetic component of the glossopharyngeal nerve (CN IX) supplies presynaptic
secretory fibres to the otic ganglion and post-synaptic parasympathetic fibres are
conveyed from the ganglion to the gland within the auriculotemporal nerve
- sympathetic comes form cervical ganglia through the external carotid nerve plexus on the external carotid artery.
what is freys syndrome?
Frey’s Syndrome or gustatory sweating can occur when a penetrating wound damages both
the auriculotemporal and great auricular nerves, and parasympathetic secretomotor fibres
from the former regenerate into the latter, eventually reaching sweat glands or blood vessels in
the skin and innervating them inappropriately. When a sufferer prepares to eat, beads of perspiration on
and/or flushing of the skin over the parotid gland accompany salivation. It is very common following
parotid surgery, and has been associated with children delivered using forceps.
the auriculotemporal and great auricular nerves, and parasympathetic secretomotor fibres
from the former regenerate into the latter, eventually reaching sweat glands or blood vessels in
the skin and innervating them inappropriately. When a sufferer prepares to eat, beads of perspiration on
and/or flushing of the skin over the parotid gland accompany salivation. It is very common following
parotid surgery, and has been associated with children delivered using forceps.
form where does the facial nerve arise?
what does it comprise?
though whcih canal does it go and what does happen in there?
what branch does it give off and werhe does it synapse?
what other two branches does it give off?
though whcih foramen does it exit?
what fibres does the cauda tympani carry?
what does it comprise?
though whcih canal does it go and what does happen in there?
what branch does it give off and werhe does it synapse?
what other two branches does it give off?
though whcih foramen does it exit?
what fibres does the cauda tympani carry?
-pontomedullary angle of the brainstem
-a large motor root and a smaller sensory root – the intermediate nerve.
- the internal acoustic meatus. They enter the facial
canal in the petrous part of the temporal bone and fuse to form the facial nerve proper.
-nerve then enlarges to form the geniculate ganglion,
-gives off the greater petrosal nerve which carries preganglionic parasympathetic fibres to the pterygopalantine ganglion.
- giving off the nerve to stapedius and the chorda tympani before exiting the skull through the stylomastoid foramen,
located between the mastoid and styloid processes.
- The chorda tympani carries taste fibres
from the anterior two thirds of the tongue and preganglionic fibres destined for the
submandibular region
-a large motor root and a smaller sensory root – the intermediate nerve.
- the internal acoustic meatus. They enter the facial
canal in the petrous part of the temporal bone and fuse to form the facial nerve proper.
-nerve then enlarges to form the geniculate ganglion,
-gives off the greater petrosal nerve which carries preganglionic parasympathetic fibres to the pterygopalantine ganglion.
- giving off the nerve to stapedius and the chorda tympani before exiting the skull through the stylomastoid foramen,
located between the mastoid and styloid processes.
- The chorda tympani carries taste fibres
from the anterior two thirds of the tongue and preganglionic fibres destined for the
submandibular region
as the facial nerve emerges form the stylomastoid foramen, what does it give off immediatly?
as the main trunk coontinousk what else does it give off?
what does it divide into in the parotid gland?
what does the facial plexus give off?
as the main trunk coontinousk what else does it give off?
what does it divide into in the parotid gland?
what does the facial plexus give off?
posterior auricular nerve, which passes posterosuperior to the auricle of the ear to supply the auricularis posterior muscle and the occipital belly of the occipitofrontalis muscle.
gives off a branch to the posterior belly of the digastric muscle
and the stylohyoid muscle before entering the parotid gland.
divides into upper t mporofacial and lower cervicofacial branches which branch and anastomose further to form the parotid plexus of the facial nerve.
The plexus gives rise to the five terminal
branches of the facial nerve which emerge from the superior, anterior and inferior margins of the
gland as the temporal, zygomatic, buccal, marginal mandibular and cervical branches.
gives off a branch to the posterior belly of the digastric muscle
and the stylohyoid muscle before entering the parotid gland.
divides into upper t mporofacial and lower cervicofacial branches which branch and anastomose further to form the parotid plexus of the facial nerve.
The plexus gives rise to the five terminal
branches of the facial nerve which emerge from the superior, anterior and inferior margins of the
gland as the temporal, zygomatic, buccal, marginal mandibular and cervical branches.
what does the marginal mandibular nervge supply3?
what does the cerical branch supply 1?
what does the cerical branch supply 1?
TIt supplies muscles of the lower lip and chin (depressor anguli oris, depressor labii inferioris and mentalis).
The cervical branch of the facial nerve also emerges from the inferior margin of the parotid
gland and passes posterior to the mandible to supply platysma.
Injuries to branches of the facial nerve result in (usually unilateral
The cervical branch of the facial nerve also emerges from the inferior margin of the parotid
gland and passes posterior to the mandible to supply platysma.
Injuries to branches of the facial nerve result in (usually unilateral
what is bells palsy?
cuase?
cuase?
Injuries to branches of the facial nerve result in (usually unilateral) paralysis of
the facial muscles (Bell’s palsy), with or without loss of taste on the anterior
two thirds of the tongue, or altered secretion of the lacrimal and salivary glands.
Common causes of facial nerve palsy include inflammation of the nerve (usually as a
result of viral infection), fracture of the temporal bone and parotidectomy (although branches of the nerve
can be identified by electrical stimulation during surgery)
the facial muscles (Bell’s palsy), with or without loss of taste on the anterior
two thirds of the tongue, or altered secretion of the lacrimal and salivary glands.
Common causes of facial nerve palsy include inflammation of the nerve (usually as a
result of viral infection), fracture of the temporal bone and parotidectomy (although branches of the nerve
can be identified by electrical stimulation during surgery)